

Sandra Bush had no idea what was about to happen when her son, Ben, stood in their living room, samurai sword in hand, and stared at her blankly. Reality had been slipping away from Ben Bush in 2017. He was 33 years old and struggled with mental illness much of his life. His mother had seen Ben's delusions snowball before.
There was a cycle: Ben's psychosis would worsen, sometimes the police would get involved, then he would go for a short and ultimately unhelpful stint in a local mental health facility. The police were frequent visitors at the Bushes' home in Hutto, a suburb northeast of Austin. Ben, at 6-foot-1 and 260 pounds, managed to keep a good relationship with law enforcement. Sandra would bring the officers donuts.

Benjamin Bush (Family Photo)
But that November, Ben's mental decline reached a climax that would change the trajectory of his life. He was hearing voices. He thought he had three wives coming to visit, and that the federal government had paid him $500 million for busting a drug ring. Sandra finally told Ben there was no money, and he snapped.
"That's when he stood up and just stared through me. I can't explain it unless you have a cat or something stares at you before they swat you in the face," Sandra said. "I didn't know what he was going to do."
Ben's brother, Philip, called 911. The panic and fear were audible in his trembling voice as he urged the police to hurry, and he watched his mother run out the front door.
Nobody was injured in the incident. Ben never took the sword out of its sheath, but his threat of violence opened the door for a felony charge of aggravated assault. According to Sandra, the police said they could charge Ben with the second-degree felony, and he would be sent to a state mental hospital for treatment.
Ben and Sandra saw a prolonged stay in a state hospital as his best shot at improving. If he could stay in treatment long enough to get stabilized, maybe Ben could turn his life around.
"I had to find a different way to get help. I knew I had a problem," Ben said. "I just didn't know how to fix it, until I found out I could go to the mental hospital for a lot longer time. Not that I wanted to get charged with anything."

Ben was booked into the Williamson County Jail and was soon declared mentally incompetent to stand trial. A judge ordered him to be sent to a state hospital.
In Texas, defendants must be able to understand the charges against them and assist in their own defense. If they can't, they're sent to a state hospital for competency restoration, which involves medication and therapy. Once stable, they're returned to jail to face the criminal justice system.
Despite the judge's order, Ben wouldn't be sent to the state hospital for months. Nobody had explained to Ben and Sandra that Texas' state hospitals were full. There were no spare beds. Ben was put behind hundreds of people on the state's waitlist, and the hospitals were admitting two or three people per day, Sandra said.
"The analogy is, we've got a guy in jail bleeding to death and a doctor saying, 'Well, we're all filled up at the moment. He'll just have to keep bleeding,'" said Keith Hampton, a criminal defense attorney who represents mentally ill defendants on the waitlist. "If you're dedicated to restoring these people's health, you don't say, 'We'll get to you in a year. Just stay in the waiting room, and your waiting room is a jail cell.'"
Since Ben's time on the waitlist, that backlog of people, locked in limbo across the state, has reached historic levels. Efforts to fix the problem have not reversed the trend, and a costly rebuild of the state's mental hospitals may not meet demand and won't be complete for years.
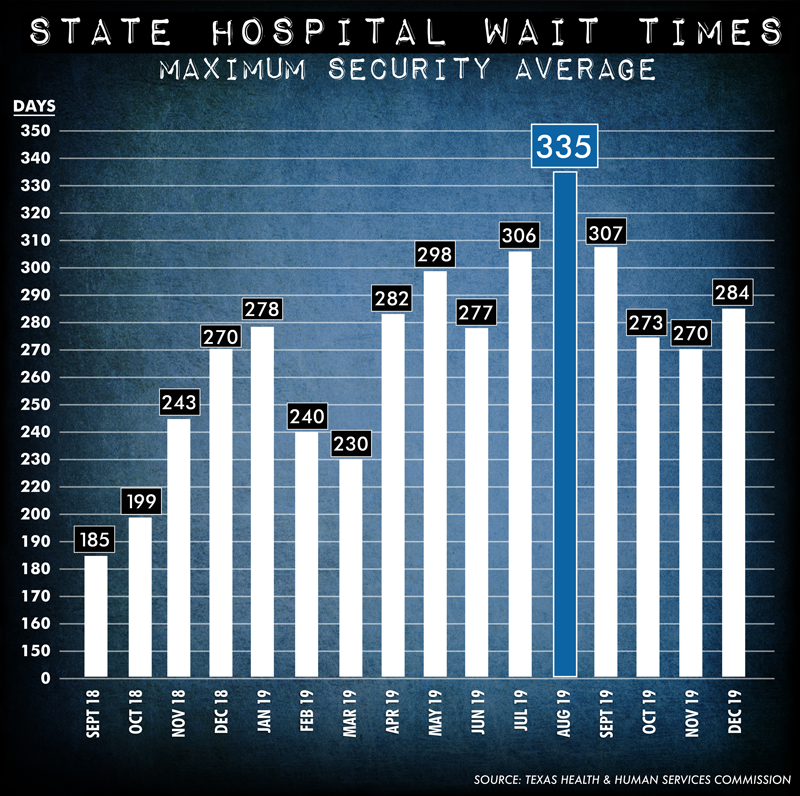
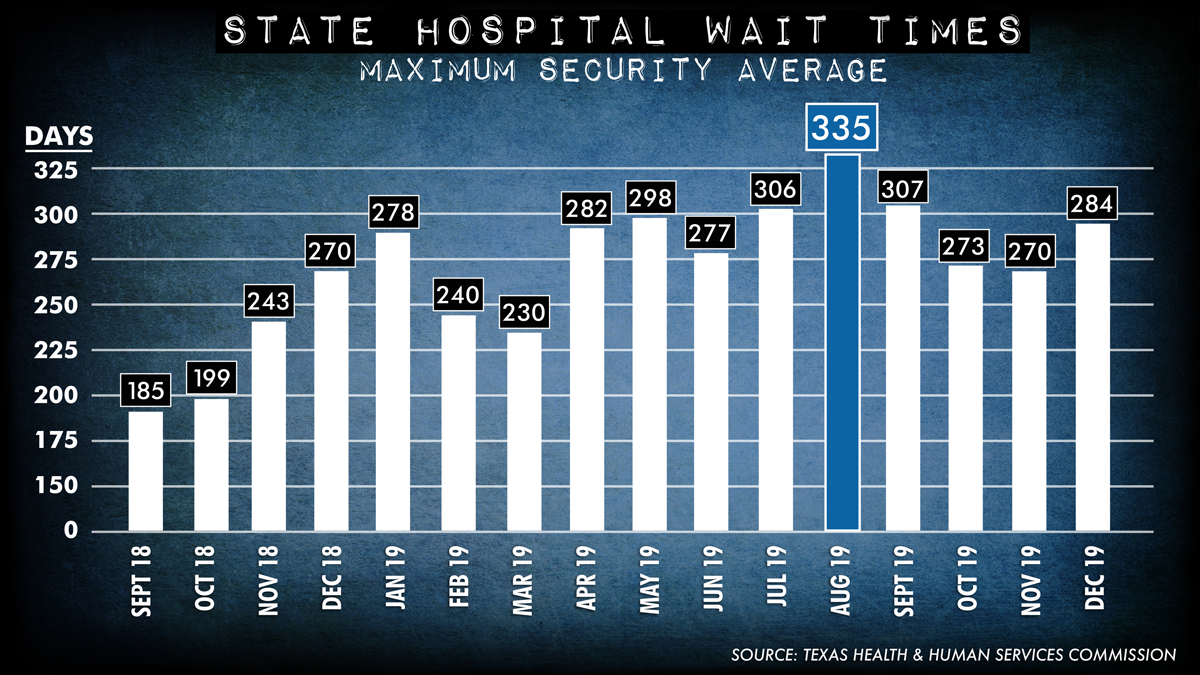
The average number of maximum security inmates in Texas' county jails waiting for state hospital beds never dropped below 230 days in 2019, peaking in August with 335 days.


The Health and Human Services Commission divides its waitlists for people charged with crimes into two categories: maximum security for potentially violent people and non-maximum security for everyone else. By 2020, there were 970 people on both lists combined, and wait times for more scarce maximum-security beds exceeded a year in some cases.
Texas officials have seen this predicament building for years.
In 2014, the state hired consulting firm CannonDesign to study the hospital system and waitlist. That study found Texas needed roughly 1,300 more state hospital beds.
A 2016 report by HHSC's Joint Committee on Access and Forensic Services, which monitors the waitlist, said the backlog had reached a "crisis levels" and the state would need 1,800 more beds over the next eight years.
"The consequences of this are visible on the pages of our daily newspapers: individuals in crises, increased costs to the State and local governments, suicides in county jails and in the community, and stress to families," according to the 2016 report.
In response, state leaders have pushed through $745 million to rebuild and expand the state hospital system. Legislators expect to complete funding in next legislative session and bring the total to more than $1 billion.
But for all that money, the state will add just 350 total beds to its current stock of 2,269. With current demand, HHSC would still be 555 beds short, according to HHSC data.
"People have been frustrated by that because it's like, 'Why aren't you building bigger hospitals?'" said Karen Ranus, executive director of the National Alliance on Mental Illness - Central Texas, which works to improve the lives of people with mental illness.
Meanwhile, tough-to-handle mental health cases strain jails, where mentally ill inmates are often placed in solitary cells and spiral further into mental illness, Ranus said.


Advocacy groups, such as the NAMI's statewide branch headed by Greg Hansch, have worked to reduce wait times and help people stuck on the waitlist.
"We speak up on these issues because we see people suffering behind bars," Hansch said. "Many of these folks are low income from broken homes, aren't able to get a good criminal defense attorney to sort of advocate for them in the legal system."
Part of the problem, Hansch said, is the state's aging state hospital buildings. For instance, Austin State Hospital opened in 1861, when it was called the Texas State Lunatic Asylum.
Demand for mental health services has increased with the state's population, and the supply of hospital beds is "just not enough," he said.
And waiting for a state hospital bed may violate a person's constitutional protection to access to a fair trial, Hansch added. In 2007, a lawsuit brought by advocacy group Disability Rights Texas against the Department of State Health Services, which oversaw state hospitals at the time, challenged the legality of extended wait times.
In that case, Disability Rights prevailed in Travis County district court. For a short period of time, people had to get a bed within 21 days or the state could be held liable, Hansch said. That requirement is not currently in effect because the judgement was overturned on appeal, according to court records.
"We'd like to see the state held accountable for ensuring that people are getting access to services in a timely fashion," Hansch said.
In fact, he added, the state is again fighting a lawsuit over the constitutionality of the waitlist.


In July 2016, Disability Rights Texas filed a class action lawsuit against HHSC in federal district court, on behalf of several county jail inmates placed on the waitlist for extended periods. HHSC now operates the state hospital system.
"Individuals with mental illness suffer needless deterioration of their mental health as they wait in jails, frequently in prolonged isolation," the lawsuit states.
Each of the plaintiffs in the case was placed on the waitlist, several for over 50 weeks. That should not happen, according to the lawsuit. The state is obligated to provide state-mandated restoration services and failing to do so is a violation of the incompetent detainees' right to due process guaranteed in the Fourteenth Amendment, states the lawsuit, which remains pending.
HHSC declined an interview for this report, citing the ongoing litigation.


For Ben Bush, the three and a half months in the Williamson County Jail were more than a possible constitutional violation. They were a life and death struggle.
"It was hard the whole way through. I don't know how I made it. There were fights every day," Ben said. "There were murderers, rapists, all kinds of stuff. Horrible things."
Like many incompetent defendants, Ben was placed in a solitary cell most of the time and got "cabin fever."

Williamson County Jail (KXAN Photo)
"There were people in there losing their minds because they didn't know what else to do," he said.
One of those individuals was Daniel Lee Charles McCoy, whose jail stay overlapped with Ben's.
McCoy, 24 and schizophrenic, was booked just weeks before Ben in October 2017 for misdemeanor assault. McCoy was found incompetent to stand trial and ordered by a judge to be taken to a state hospital for treatment. Like Ben, he was placed on the waitlist. McCoy would have to wait eight months to get a state hospital bed.
He never made it.
McCoy steadily deteriorated during his stay. As the months wore on, he displayed worsening psychotic behavior, according to a federal lawsuit filed this year by McCoy's mother against Williamson County and a handful of jail employees.
McCoy was found yelling at "demons," smashing his head against a cell door and eating the padding from a cell wall. Toward the end, McCoy had been eating his own excrement, bodily fluids and bacterial scum in his toilet. He had lost his mind, and Williamson County jailers did little to help him, according to the lawsuit. Williamson County officials declined an interview.
About five months after being booked, McCoy was found unresponsive on his cell floor with white and red foam coming out of his mouth, the lawsuit states. He was taken to Ascension Seton Williamson Hospital where doctors diagnosed him with a slew of critical problems, including aspiration pneumonia, cardiac arrest and respiratory failure. Five days after admission, McCoy was removed from life support and died.
Williamson County "continued to house Daniel in a cell which was essentially a metal box, with a single window. This increased Daniel's anxiety, anti-social behavior, psychotic episodes, and mental anguish and emotional distress," according to the lawsuit. "Daniel suffered a completely unnecessary and horrific death in the Williamson County jail."


Sandra Bush didn't know about McCoy, but she knew her own son was suffering in jail during that time. She scrambled daily to find a way to get Ben out.
"Every day it was just like, 'What can I do today... to get him out of there?'" Sandra said. She began writing letters to congressmen, senators, even the president.
"Nobody wanted to listen to me," she said.
Then she found the Texas Jail Project, a nonprofit that provides resources to the families of incarcerated people. Diana Claitor, TJP's executive director, worked with Sandra to urge Ben's public defender to file a writ of habeas corpus that would compel HHSC to open a bed for Ben. Claitor has directed numerous people to use the writ. Her organization has a webpage dedicated to educating people on the procedure. Ben "never should have been in that situation," she said.
"We learned a lot about his case and the flaws in the system," Claitor added. "Every case like this points to a different aspect of the system that isn't working."
That writ, originally composed by Keith Hampton about 15 years prior, would help speed up Ben's removal from county jail. Hampton did not represent Ben, but his writ has been circulated around the state and used by numerous attorneys, he said.
Hampton said he's proud the writ has helped so many incompetent people get out of county jail. To be found incompetent, he said, these people must have "profound mental illness," and they need to be in a hospital.
"To be competent, all you have to be able to do is to have a rational understanding that you're in court and that the lawyer is your lawyer and not a robot or some other delusion," Hampton said.
After the writ was filed in Ben's case, he was moved to North Texas State Hospital at Vernon, one of only two state hospitals that admit maximum-security individuals. He was later transferred to Kerrville State Hospital, which houses nonviolent defendants. Overall, he spent seven months in the state hospital system, which was the longest continuous period he had received mental health treatment. He was prescribed new medication, and he improved. A year after he was arrested, Ben's charges were dismissed, in the "interests of justice," according to court records.
Ben credits his progress, in large part, to staying on his medication. But many people locked in county jails don't have the option to keep taking their medications. Some jails don't provide the same medicine given at state hospitals, said Hansch.
"The medications that are available in jail, and other services that are available in jail, don't match what they were receiving in the state hospital system," Hansch said. "They're going from a pretty high level of care in the state hospital system to a pretty low level of care in jail."
When stabilized defendants are moved back to jail and taken off the state hospital prescriptions, the results can be crushing.




Maria Anna Esparza had no idea what was happening when she heard gunfire early on the morning of May 27, 2011. Bullets hit her front door, the roof and a back wall. She soon learned it was her son, Adan Castaneda, delusional and shooting wildly from the end of the driveway.
Investigators placed evidence markers over 23 shell casings strewn across Maria Anna's driveway after Adan fired at the family's home. (Comal County)
Maria Anna knew her son was not well. Adan, a 25-year-old former staff sergeant and Marine scout sniper, had been sinking further into mental illness since he was discharged from the military in 2008. War, combat, explosions, death and PTSD had taken their toll.
"He was stationed in Iraq, and he saw many things that people don't get to see in their lifetime, or don't wish to see, that impacted him," Maria Anna said. "And so when he came back, he was not the same young man that left."
Circumstances outside Adan's control, including the murder of his brother shortly after his military release, worsened his mental state.
In that March 2009 incident, Adan's brother, Alonzo Garza, and a group of friends were hanging out late at a home in Schertz, northeast of San Antonio. A partygoer randomly shot and killed Garza, and Adan awoke to find his brother in pool of blood in the kitchen. From that point, Maria Anna said her son began losing control.
"I can't tell you that there was any one trigger... when you don't manage the things in your life that you can't comprehend, then you have an explosion at some point," Maria Anna said. "He just had a huge explosion."
Two years later, tormented by mental illness, Adan drove to the family's home at 4 a.m. and fired 23 bullets at the house. No one was injured, but the Comal County district attorney prosecuted aggressively. Adan was slapped with seven felony charges, including two counts of attempted murder and aggravated assault with a deadly weapon. He was even charged with tampering with evidence for tossing the magazine from his .45 caliber Glock pistol into the grass while police arrested him at gunpoint. He faced the possibility of life in prison.
Months after being booked in the Comal County jail, Adan was found incompetent to stand trial and ordered to be sent to North Texas State Hospital. Maria Anna was hopeful.
"I felt a great sense of relief, thinking, 'Oh, you know, finally he's going to get some help,'" she said. "I waited a couple of weeks, and nothing happened."
Maria Anna called the sheriff's office to ask about the transfer; they told her to call the hospital. A woman with the state hospital system finally informed Maria Anna there was a waitlist, she said.
"She looked it up and said, 'Well, it'll be eight months to a year.' And I was shocked, and I asked, 'How could that be?' And she said, 'I just don't have enough beds,'" Maria Anna recounted. "That's when I realized that, you know, he wasn't going to get the help that he needed, and that sense of relief was false, and I just was pretty lost."
Adan spoke with KXAN by phone about his time in Comal County. He said it's particularly difficult for mentally ill people, who aren't making rational and logical decisions, to stay safe in jail.
"People prey on you... take advantage of you, take food from you," he said. "There's a lot of predators and gang members."
Maria Anna was desperate for help getting her son into a state hospital. With the help of an advocacy organization, she found Keith Hampton. Hampton told Maria Anna she needed to file a writ to get her son into a state hospital, and he helped her find an attorney to file it. Maria Anna later hired Hampton to defend her son at trial.

Adan Castaneda (Family Photo)
Adan ultimately spent four years pretrial, including two loops through the state hospital system and 1,100 days alone in a county jail cell. After being stabilized a second time, he was returned to Comal County jail and waited 15 months for trial. During that time, his mental illness began resurfacing. He was on the verge of decompensating again and heading back to the state hospital a third time, but he managed to make it through is trial, Hampton said.
"If you're mentally ill, you can find yourself in a kind of a dark Groundhog Day, you know, experiencing it again and then again and then again," Hampton said.
In 2015, nearly four years after his initial arrest, Adan was found not guilty on four charges. He was found not guilty by reason of insanity of the remaining three charges, which means he will be under the court's jurisdiction until 2031. He is reviewed yearly to determine if he needs to be committed for mental health treatment, Maria Anna said.
Maria Anna explained how she has been the one constant through it all, fighting against federal, state and local bureaucracy. She lost one son, she said, and she couldn't lose another.
"I am very thankful that nothing happened the day that I lost my mind, and no one got hurt. She's been there. She's been supportive," Adan said. "It's been difficult, but, you know, we're managing, and I think things are going to be okay."


To reduce the wait list, and the number of cases like Adan's, Ranus said the state will have to get creative if it isn't going to build enough bed space to meet the current level of demand.
That means diverting more people before they enter the criminal justice system, and better utilizing beds already in the community, like private hospital beds. Diversion programs, for example, can allow lower-risk defendants to stay in the community, receive treatment and undergo periodic monitoring. Each successful diversion can take pressure off the state hospital waitlist.
"How do you change the system so that you create opportunities for people to get help earlier... before they're in that crisis stage where they're breaking into some place or they're doing something that causes and triggers some kind of incarceration?" Ranus asked.
State Sen. Charles Perry, R-Lubbock, has pushed for reforms to improve competency restoration wait times in the Legislature. He said the state has put ample money toward rebuilding the state hospital system, but more effort needs to be placed on finding cheaper ways to create space for people on the waitlist.
"The number one thing we have to do today, in my estimation, is to continue to find a way to fund bed space," Perry said. "There are valid solutions and opportunities to do that very thing... it's all expensive, but without breaking the bank."
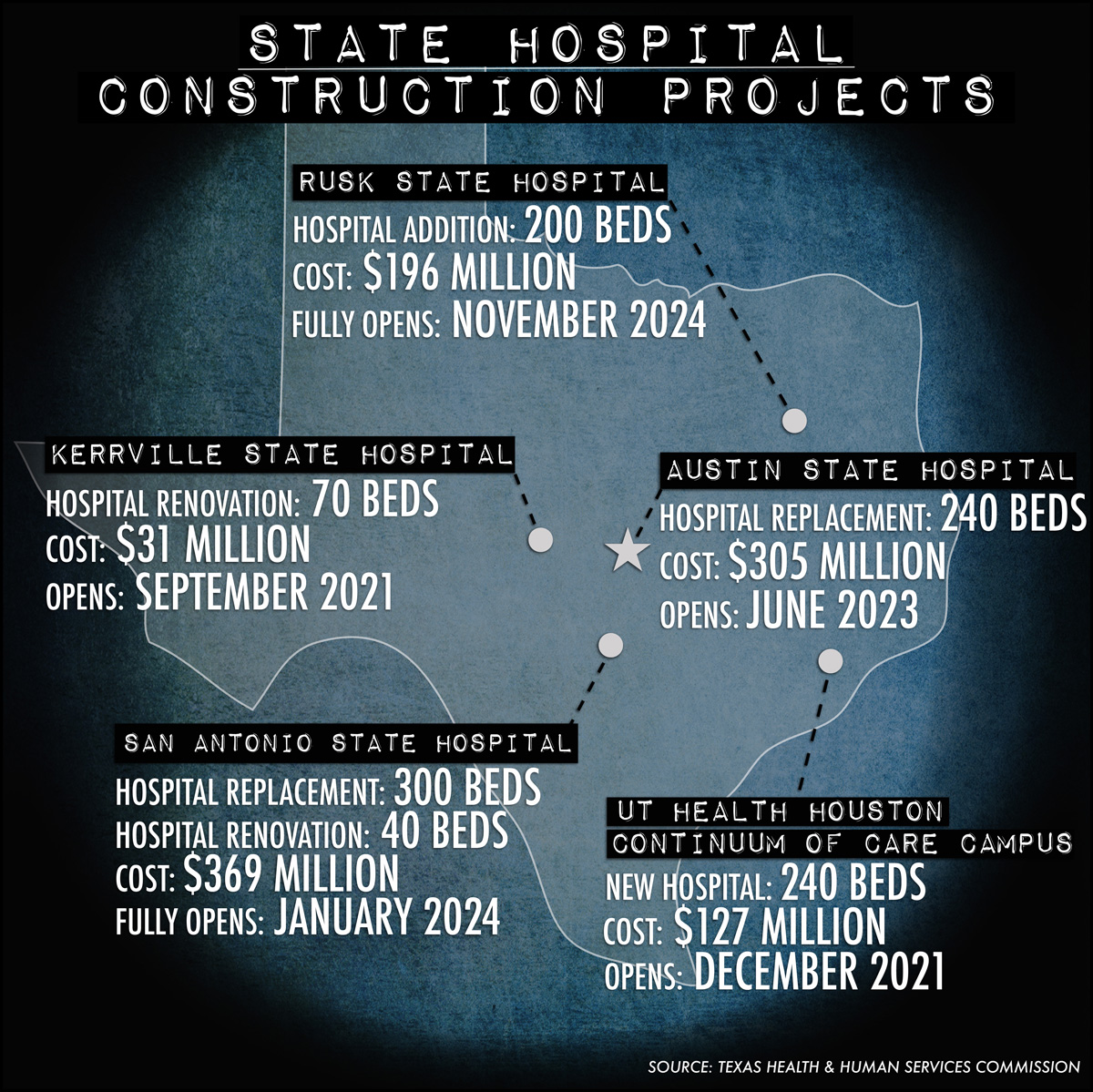

The Texas Legislature invested more than $750 million for a first round of construction on state hospitals. The Health & Human Services Commission will seek funding in 2021 to complete the projects, designed in partnership with medical schools and community providers.
The state could repurpose existing structures to create more bed space, he said. For rural areas lacking access to mental health facilities and psychiatrists, like his 51-county West Texas district, the state must fund and provide tools to local mental health authorities. For example, telepsychiatry — which allows a provider to remotely assess a person via camera and screen — gives jails more and faster access to professionals to determine a person's competency, he said.
Much of the funding for state hospital construction has gone to urban areas, but those improvements are not easily accessible for people having a mental health crisis in Lubbock or Tahoka, he said.
Improvements already underway include adding maximum-security beds to Kerrville State Hospital, replacing 240 beds at Austin State Hospital, and building a new 240-bed hospital at the UT Health campus in Houston for short-term stays, according to HHSC.
Recently retired State Sen. Kirk Watson, D-Austin, has advocated for funding the state hospital rebuild and revamping the Austin State Hospital.
Watson said the state hospital improvements will help provide a "continuum of care," which includes carrying a person's mental health care through each stage of the criminal justice process.
"There is no question the state needs more beds," Watson said. "But there's also no question that one of the ways to approach this that may be better for everybody involved... is to look at aspects beyond building a bed."
That could include ensuring the same medications in jail as those at the state hospital. It could also be a smoother transition between inpatient and outpatient mental care facilities. And with higher quality hospitals, the state should be able to provide more efficient care. Texas could also reduce the deadline for the length of time required for competency restoration, Watson said.
Watson has also advocated for providing competency restoration services outside the confines of state hospitals.
In the 2017, he coauthored Senate Bill 292, which created an HHSC grant program to fund local mental health authority programs to reduce recidivism and wait times for the state hospitals. More than $108 million has been put into the grant programs. Of the state's 39 local mental health authorities, four have created in-jail competency restoration programs, according to HHSC records obtained by KXAN.


But despite the state's push to fund it, many experts, including county jail officials like Danny Smith, director of inmate health programs with the Travis County Sheriff's Office, have resisted in-jail competency restoration.
"We just don't feel that jail-based competency restoration is the right way to do it." Smith said. "We're talking about treating mental illness, which is a disease, and a disease should be treated in a hospital, not in a jail."
Smith said Travis County defendants were waiting up to 400 days for a maximum-security bed and roughly 90 days for a minimum-security bed in February. Those wait times are stretching the jail's resources.

At Travis County Correctional Complex in Del Valle, one officer typically monitors a 48-person unit. The mental health unit requires triple the number of officers, Smith said.
"It's very difficult for an individual to remain in jail and to have a positive attitude and not to get worse, to decompensate," he said. "Unfortunately, some people end up getting additional charges because the level of agitation they have is so high. They end up assaulting someone."
Smith said Travis County has the funding to provide the same medications as a state hospital. The county also has a full-time psychiatrist and four nurse practitioners assisting with treatment.
But many counties don't have those resources. Even at the state level it is difficult to retain medical professionals in state hospitals.
"We don't have enough psychiatrists, psychologists, psychiatric nurses in the state of Texas," Ranus said.


In April 2019, plaintiffs' attorneys in the ongoing class action case against HHSC deposed Mike Maples, the commission's deputy executive commissioner for the health and specialty care system. In transcripts obtained by KXAN, Maples explained HHSC's struggled to recruit enough staff to overcome attrition.
Maples didn't say exactly why the hospital system struggles with retention, but he offered some examples. For one, the work is difficult. Another hurdle: the hospitals are in remote areas. Compensation could also be an issue, he said.
"Reasons why people don't apply to our jobs, I'm assuming, I just stopped at a Buc-ee's [a large convenience store] yesterday, it pays $3 more an hour with benefits and retirement. That's my competition. So I can only assume the reason why they're not applying is pay and benefits and those type things," Maples said in the deposition.
Maples' statements reveal HHSC's monumental task. Without enough funding, the agency can't maximize state hospital space. But it's a struggle to find people to do such stressful work, regardless of the funding.
And even if the system is working well, and inmates are being mentally restored and returned to their counties to face trial, the wheels of justice often turn slowly.
For so many reasons, it's tough to cycle people through the system to free up space. However, when people finally get a spot, it can be life changing. For Ben Bush, the state hospital was his last option.

Sandra and Ben Bush (KXAN Photo)
Ben and his mother Sandra recounted the horrors of the waitlist and jailtime from their cramped living room stacked with boxes. Ben often sleeps through the day on a living room sofa with trash bags covering the cushions. Sandra's health has been deteriorating. Ben's father died last May, and the financial strain pushed the family to move from Hutto to a duplex on the outskirts of Waco. Each day is a struggle.
Ben is finally staying steady on more than half a dozen medications, but the pills have difficult side effects. During our interview, he dozed off twice at the dining room table. He's been home, and out of the criminal justice system, for a year and a half.
Since he got back from the hospital, Ben has been able to do something he struggled with for years: stay on his medication. He credits his months in Vernon and Kerrville for the improvement. He is no longer delusional. He can think straight, and he has ambitions. Ben even started a GoFundMe page in hopes of raising money for a private mental health hospital.
In hindsight, with Ben's progress, Sandra said she's happy to have her son back. But the aggravation and stress of the experience was nearly too much to take.
"I just hope they do something in a hurry and people become aware of it, because it's a horrible problem," Sandra said. "Benjamin's not the only one. I mean, there's people all over the state that have the same type of story."